 |
FIG. 1 - Vertical line of gravity. As far as we know this is one of the first drawings of the vertical line of gravity of the standing man, printed in the book of Borelli «De motu animalium» (1680). |
Introduction
During
millennia, man stood upright without asking questions about the
machinery that allows this posture. The idea of an animal machine
was unknown, moreover. But when he dared notice that celestial
bodies were submitted to the laws of the mechanics, then he began
thinking his own body in terms of masses, accelerations, forces,
balance (Borelli, 1680) (fig. 1)...
 |
FIG. 1 - Vertical line of gravity. As far as we know this is one of the first drawings of the vertical line of gravity of the standing man, printed in the book of Borelli «De motu animalium» (1680). |
The spiral of questions about upright posture was in
being then; actually it was initiated by Charles Bell at the beginning
of XIX-th century: «How does man maintain a posture upright
or tilted against the wind?» He wrote «It is evident
that he possesses 'a' sense by which he knows the tilting
of his body and that he possesses the capacity to right it and
to correct any deviation from the vertical. But what sense is
it?» (Bell Ch., 1837).
Charles Bell set the problem clearly. But he set it inside the
problematic of his century! At this time it was impossible to
imagine that a function is not assumed by an organ - the
function creates its organ - and an sense organ in this case:
«What sense is it?». The vestibular apparatus put
forward Flourens (Flourens P., 1829), and gradually his proposal
was winning. Not only the vestibule is an organ that gathers in
a definite, visible, place parts of the body in connection with
balance, but moreover this organ is structured according to the
Cartesian concept of the three dimensions space. Nothing more
was needed to seduce all the spirits... All, except one at least:
Vierordt.
Tübingen's physiologist was
aware that things were not so simple (Vierordt K., 1860, 1862,
1864, 1871, 1877). He had to recognise that looking for «THE»
sense of balance, in fact several senses had been found. He knew
that vision (Romberg M.H., 1853), sensibility of soles (Heyd,
undated), proprioception - muscles sense as it was said then -
(Longet, 1845) act also for keeping upright posture. Then how
to understand this bizarre function of the upright position, manifestly
impossible to summarise in a single organ of senses? The concepts
of system, control, cybernetics were still far from being available.
If it could not yet be understood how does man maintain an upright
posture, at least that could be observed. This remark, brilliant
of simplicity, led Vierordt to become the first posturograph in
the world. He, the first, invented a system which allowed recording
the postural sway of a man standing quiet (fig. 2), so much he
was sure that these small oscillations would introduce us to the
secrets of this endless struggle that man's body leads with gravity
forces to stabilise itself.
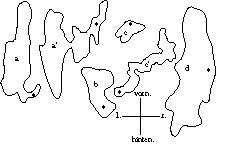 |
| FIG. 2 - First stabilometric
recordings. Vierordt kept only the envelope of the drawing made through the feather worn by the standing subject, in the eyes open (a) and closed condition (a'); in the «position hanchée», the right leg being the support (b); sitting eyes open (c) and closed (c'); standing on the only right foot (d). |
One hundred and fifty years passed by since these first
posturographic recordings and gradually it was noticed that Vierordt
was right, things are not as simple as Flourens thought. Today
all the basic researchers admit that upright posture is controlled
by a split system, which integrates sensitive and sensory information,
coming from multiple canals: visual, oculomotor, vestibular, somatosensory,
plantar exteroceptif. And we no longer have difficulties handling
these experimental data from posturography by means of models
arisen from system theories. Vierordt was right... Flourens swindled
us!
From this evolution of ideas on
postural control physicians have to draw the necessary conclusion:
we must criticise our interpretations of all the diseases, which,
by one way or another, concern standing upright quiet. The notion
of system dominates the postural physiology, let us impose it
to our reflections about the diseases of standing man. Posturographic
recordings gave evidence of their efficiency in postural physiology,
let us give evidence of their necessity for every patient who
has trouble standing upright quiet.
Clinical stabilometry
Observing the quality of the postural
control of a patient begins inevitably with a comparison of his
performances to those of a reference population composed of healthy
subjects. Is the postural control of this patient normal or not?
Such is the first question that physician must be able to answer,
and it is not evident...
| FIG. 3 - Distribution
of the parameter of surface in normal population. Histogram of the real distribution, Gaussian curve of the theoretical one. Mean: 91, 95% Limits of confidence: 39 and 210. Unity: square millimetre. N=100. |
|
For lack of consensus within the International Society
of Posturography about the standardisation of posturographic recordings
(Kapteyn et al., 1983; 7-th international Symposium, Houston,
Texas, December 2, 1983) the Association Française de Posturologie
decided to settle precise standards for clinical stabilometry
(A.F.P., 1984) concerning construction of platforms (Bizzo et
al., 1985), recording conditions and signal analysis (A.F.P.,
1985; 1986). This standardisation allows characterising postural
control of a man standing quiet by means of a series of parameters
whose statistical distribution is known. It is therefore possible
to say, in this context of standardisation, that the postural
control of a patient is normal or not. The equipment for clinical
stabilometry, normalised and computerised, corresponding to the
schedule of the Association Française de Posturologie,
is commercially available, proposed by various French or foreign
manufacturers (C.I.A. Modena; DYNATRONIC, Céreste; Q.F.P.
SYSTEM, Sophia-antipolis; SATEL, Toulouse; MIDICAPTEURS, Toulouse;
DUNE, Mulhouse).
To suspect the interest of stabilometric
recordings of patients who have trouble standing upright, an example
is better that long speeches. Low back pain was the object of
several stabilometric studies of which some are already published
(Gagey, 1986; Gagey et al., 1986; Guillemot and Duplan,
1995; Liebenson C., 1996), they will exemplify, but on the condition
of saying and saying again that the interest of stabilometry widely
extends beyond the field of low back pain.
Stabilometric study of low back pain
Knowing the position of the gravity
line of a low back pain patient allows better understanding of
the type of constraint to which his rachis is submitted and stabilometry
discovers great variations from a patient to another.
X-Mean
In the frontal plane, normal
mean position of the gravity line (X-Mean) varies in extremely
tightened limits; 10 millimetres to the right or to the left of
the median line constitute its 95 % confidence limits. Now, curiously,
only 20 % of low back pain patients (Guillemot and Duplan, 1995)
present a statistically abnormal position of their gravity line
in the frontal plane, more, for half of them this statistically
abnormal position can be connected with an orthopaedic abnormality.
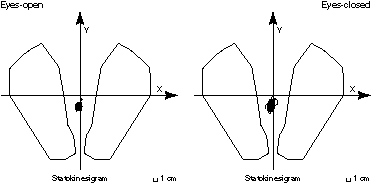 |
| FIG. 4 Stabilometric
recordings in the eyes open and closed conditions. The «spot» between the feet represents the set of the successive positions of the centre of pressure of the subject, sampled during the duration of the recording, here 51,2 seconds. The analysis of this signal supplies a series of parameters for which normal distribution is known (See fig. 3). |
So the hypothesis that low back pain would be due to
an abnormal tonic postural asymmetry, isolated, able to divert
the gravity line (Créhange, 1950), this hypothesis is not
massively supported by this statistics. However, even though there
is a few, there are low back pains, which come along with such
a tonic asymmetry. Their treatment has to take it into account.
Y-Mean
In the sagittal plane on the
other hand (Y-Mean) a much more important proportion of abnormalities
of position of the gravity line is found and always in the same
direction: 64 % of patients have a gravity line behind the backwards
95 % confidence limit of normality (Guillemot and Duplan, 1995;
Guillamon et al., 1991; Gagey et al., 1986). This
transfer of constraints towards articular processes of vertebrae
is not a big physiopathologic discovery! It has been known for
a long time that these joints may suffer during low back pain.
But the 36 % of patients who do not present this backward transfer
of their gravity line deserve certainly an adapted treatment.
Area
Normal subjects stabilise their
gravity line inside a cylinder of less than a square centimetre
of section (AFP, 1985). But one patient out of two does not manage
to stabilise his gravity line inside the 95 % confidence limits
of the distribution of this area (Guillemot and Duplan, 1995).
Why this difference? Why the precision of the postural control
system during low back pain sometimes is disrupted sometimes is
not? And is this dysfunction a cause or a consequence of the low
back pain? They disappear simultaneously, but what does that mean?
On the other hand the existence
of this dysfunction of the postural control system opens new therapeutic
perspectives: since this system works badly, we are incited to
tickle its inputs, to manipulate them, to look for the «small»
(Gagey et al., 1998c) modification which will restore a
correct functioning of the control system: systematic deviation
of the visual space in the plane of such or such semicircular
canal, change of the topology of cutaneous plantar pressure, systematic
modification of the trigeminal impulses, without forgetting the
direct manipulations of the rachis and/or its proprioceptive rehabilitation
(Gagey and Weber, 1999). When low back pain appears as one, or
in connection with one, disorder of the postural control system,
we must take advantage of that to widen our therapeutic arsenal;
it works!
Normalised amplitude in the frequency band 0,2 Hz (ANØ2)
The excursions of the gravity
centre provoked by the ventilation movements are of the same order
of magnitude as postural sway. Therefore logically ventilatory
rhythm - around 0,2 Hz - should be seen on stabilometric recordings,
spontaneously, without any trick of calculation (Bouisset and
Duchêne, 1994), but in fact it does not appear (Gurfinkel
et al., 1971; Gagey, 1986; Gagey & Toupet, 1997, 1998b)
(fig. 5A); the impact of ventilation on postural sway is compensated
by a syncinesia. But during some disorders, as low back pain for
instance, the efficiency of this syncinesia is blocked, possibly
by a postural tonic phenomenon (?), at least ventilatory rhythm
appears massively and spontaneously on stabilometric recordings
(Gagey, 1986; Gagey & Toupet, 1998a) (fig. 5B) of 46 % of
the patients, according to Guillemot and Duplan (1995).
The notion of a relationship between
rachis and breathing is not new in physical medicine but now,
thanks to stabilometry, therapeutist can notice that in fact this
relationship is implied or not in the suffering of his patient
and that is not without importance for the treatment.
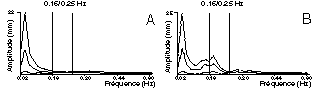 |
| FIG. 5 - Ventilatory
rhythm and amplitude of postural sway. Mean and deciles 10 and 90 of the amplitude spectra from 100 normal subjects (A) and 47 low back pain patients (B). In the frequency band that corresponds to the ventilatory rhythm, the amplitude of postural sway is weakened in normal subjects, and it is not in low back pain patients. (Gagey & Toupet, 1998a). |
The Romberg's quotient
The postural control system has
to integrate a considerable mass of information from all its inputs,
and clinical experience shows that this sensory integration is
one of the weak points of the system. Rather often one notices
that sometimes normal vestibular information is not used by the
postural system - something like a «vestibular omission»
- (Freyss et al., 1994), or sometimes normal visual information
is not integrated, the patient behaves as a blind person from
the postural point of view (Marucchi and Gagey, 1987): he is no
more stable eyes open than eyes closed. This integration of visual
information is easy to control because it is enough recording
the patient in the eyes open and eyes closed conditions and comparing
results by a quotient, the Romberg's quotient (Henriksson et
al., 1967; Van Parys and Njiokiktjien, 1976).
Now during a stabilometric study of a series of 126 low back pain, presented at the tenth Symposium of the International Society for Postural and Gait Research (Munich, September 2-6 1990), Guillamon and Gentaz noticed that evolution of this Romberg's quotient and evolution of low back pain are parallel in 90 % of patients. Values of this quotient return towards normal when pain disappears and conversely. This phenomenon is not explained yet, at least we can note that it is coherent with the place of the rachis between the two big sources of postural information. Logically the mutual position of the cephalic and plantar sensors must be known by the system so that information which result from these sensors can be used jointly. This remark of coarse robotics supplies a new track for the therapeutist, and a surprising one, who would have thought of taking charge of the integration of the visual input in the postural control during low back pain? Now this integration can be manipulated (Gagey and Weber, 1999).
Conclusion
Stabilometric studies of low back
pain are reassuring: they consolidate many common ideas (suffering
of posterior articular, role of the tonic postural asymmetry,
intricacy of the ventilatory and postural kinetics), but these
studies also show that patients do not always follow all the common
ideas, and the therapeutist in view of the results of stabilometric
recordings can modulate his treatments to adapt them to «this»
patient. Suffering from his back is only a symptom that covers
different realities and stabilometry can help us to identify them.
As for the new proposals to manipulate
the inputs of the postural system and/or their integration, their
interest asks to be validated on very great series. Currently
they have been used with a certain success only on some thousand
of patients; enough to speak about them (Gagey and Weber, 1999),
too much little so that asserting was allowed.
On the other hand, one can - and
one must - assert that upright posture is controlled by a split
system which integrates sensitive and sensory information coming
from multiple canals: visual, oculomotor, vestibular, proprioceptif,
plantar exteroceptif. One has therefore to assert that disorders
of upright posture must be observed as Vierordt did, and must
be thought with concepts of systems towards which also Vierordt
led us.
Vierordt was right, Flourens swindled
us.
References
A.F.P. (1984) Standards for building a vertical force platform
for clinical stabilometry: an immediate need. Agressologie, 25,
9: 1001-1002.
A.F.P. (1985) Normes 85. Éditées par l'Association Française de Posturologie, 4, avenue de Corbéra, 75012 Paris, France.
A.F.P. (1986) Études statistiques des mesures faites sur l'homme normal à l'aide de la plate-forme de stabilométrie clinique normalisée. I) Paramètres spatiaux. Agressologie, 27: 69-72.Bell Ch. (1837) The hand. Its mechanism and vital environment. 4th ed., V. Pickering (London): 234-235.
Bizzo G., Guillet N., Patat A., Gagey P.M. (1985) Specifications for building a vertical force platform designed for clinical stabilometry. Med. Biol. Eng. Comput., 23: 474-476.
Bizzo G. (1994) Étude dynamique de la plate-forme In P.M. Gagey et al. (Eds) Huit leçons de posturologie. Editées par l'Association Française de Posturologie, 4, avenue de Corbéra, 75012 Paris, Quatrième édition.
Borelli (1680) De motu animalium. Bernado (Rome)
Bouisset S., Duchêne J.L. (1994) Is body balance more perturbed by respiration in seating than in standing posture? NeuroReport 5: 957-960.
Créhange P.A. (1950) Ulcère variqueux. Étiologie, Traitement. Maloine, Paris.
Flourens P. (1829) C.R. Acad. Sci. (Paris)
Freyss G., Freyss M., Sémont A., Vitte E., Miron C., Diard J.P. (1994) L'équilibre du sujet âgé; apport des explorations instrumentales; aspects particuliers aux atteintes vestibulaires; prise en charge de ces malades, In: Vertiges 93. G.E.V., Arnette, Paris, 115-164
Gagey P.M., Gentaz R., Guillamon J.L. (1986) L'examen postural du lombalgique. Revue de Médecine du Travail, 13, 2 : 48-50.
Gagey P.M. (1986) Postural disorders among workers on building sites. In Bles W., Brandt Th. (Eds) Disorders of posture and gait. Elsevier (Amsterdam): 253-268.
Gagey P.M., Gentaz R. (1996) Postural disorders of the body axis. in Craig Liebenson (Ed.) Rehabilitation of the spine. Williams & Wilkins, Baltimore, ISBN 0-683-05032-X, 329-340.
Gagey P.M., Toupet M. (1997) Le rythme ventilatoire apparaît sur les stabilogrammes en cas de pathologie du système vestibulaire ou proprioceptif. in Lacour M., Gagey P.M., Weber B. (Eds) Posture et Environnement. Sauramps, Montpellier, 11-28.
Gagey P.M., Toupet M. (1998, a) Étude des oscillations posturales anormales dans la bande de fréquence 0,2 Hetz. Y a-t'il une pathologie infracanaliculaire? in Lacour M. (Ed) Posture et Équilibre. Sauramps, Montpellier, 29-42.
Gagey P.M., Toupet M. (1998, b) L'amplitude des oscillations posturales dans la bande de fréquence 0,2 Hertz: Étude chez le sujet normal. in Lacour M. (Ed) Posture et Équilibre. Sauramps, Montpellier, 155-166.
Gagey P.M., Martinerie J., Pezard L., Benaim Ch. (1998, c) L'équilibre statique est contrôlé par un système dynamique non-linéaire. Ann. Oto-Laryngol., 115: 161-168.
Gagey P.M., Weber B. (1999) Posturologie; Régulation et dérèglements de la station debout. Deuxième édition. Masson, Paris.
Guillamon J.L., Gentaz R., Baudry J. (1990) The postural disturbances induced by low back pain. 10th International Symposium of the Society for Postural and Gait Research. Münich, September 2-6 1990. (Communication non publiée).
Guillemot A., Duplan B. (1995) Étude de la prévalence des troubles posturaux au sein d'une cohorte de 106 patients lombalgiques. In: Gagey P.M., Weber B. Entrées du système postural fin. Masson, Paris: 71-77.
Gurfinkel V.S., Kots Y.M., Paltsev E. (1971) The compensation of respiratory disturbances of the erect posture of man as an example of the organization of interarticular interaction. In: Gurfinkel V.S., Fomin S.V., Tsetlin M.L. (Eds) Models of the structural functional organization of certain biological systems. MIT Press, Cambridge: 382-395.
Henriksson N.G., Johansson G., Olsson L.G., Ostlund H. (1967) Electric analysis of the Romberg test. Acta Otolaryngol. Suppl. (Stockh.) 224: 272-279.
Heyd (cité par Vierordt, 1877 sans références)
Kapteyn T.S., Bles W., Njiokiktjien Ch., Kodde L., Massen C.H., Mol J.M.F. (1983) Standardization in platform stabilometry being a part of posturography. Agressologie, 24, 7: 321-326.
Longet F.A. (1845) Sur les troubles qui surviennent dans l'équilibration, la station et la locomotion des animaux après la section des parties molles de la nuque. Gazette Médicale de Paris, 13: 565-567.
Marucchi C., Gagey P.M. (1987) Cécité posturale. Agressologie, 28, 9: 947-949.
Romberg M.H. (1853) Manual of nervous diseases of man. (Trad. anglaise) Syndenham Society, London.
Van Parys J.A.P., Njiokiktjien Ch. (1976) Romberg's sign expressed in a quotient. Agressologie, 17, B: 95-100.
Vierordt Karl von (1860, 1862, 1864, 1871, 1877) Grundriss der Physiologie des Menschen. H. Laupp, Tuebingen.